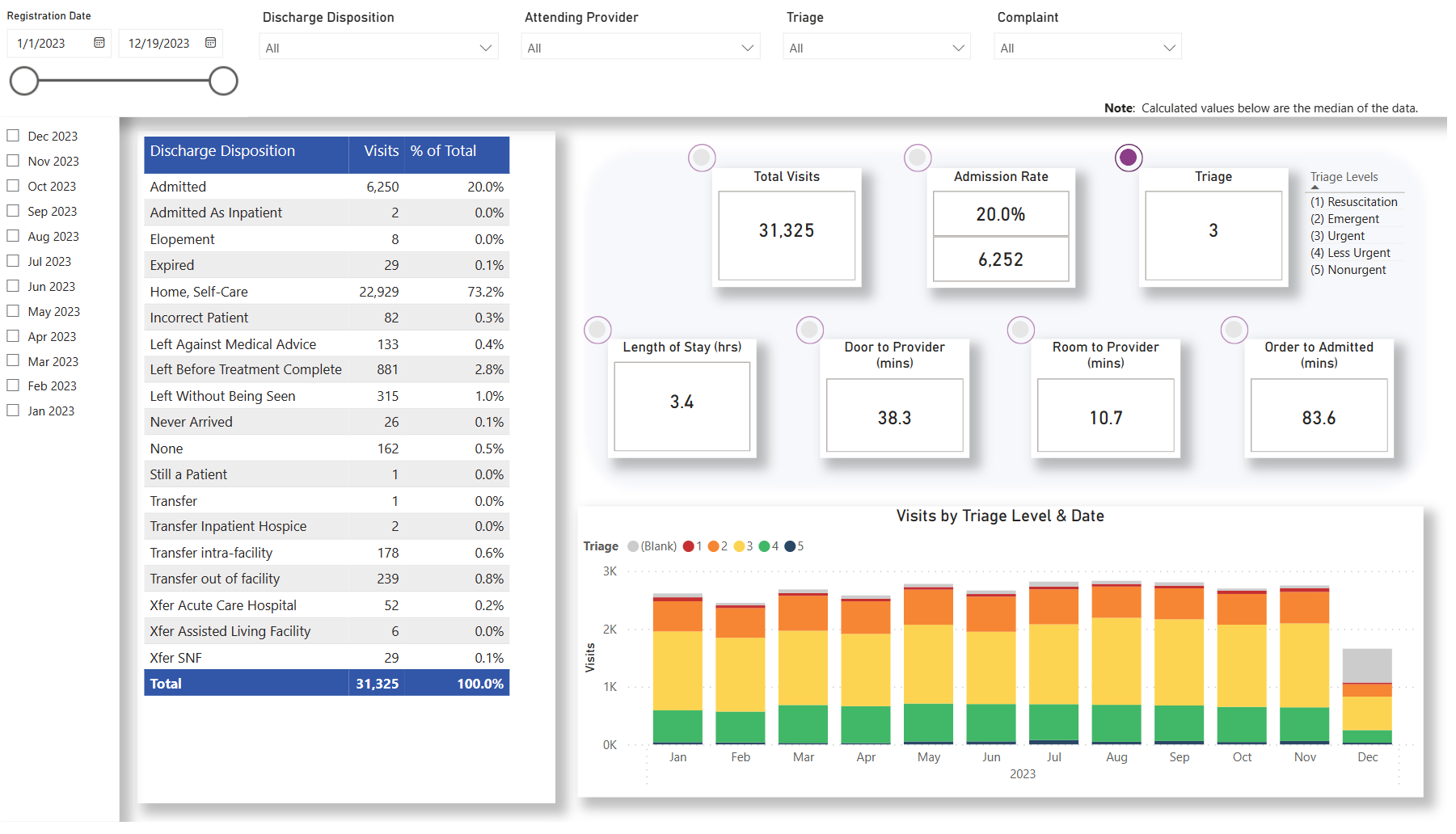
If your electronic Clinical Quality Measure (eCQM) performance numbers do not reflect your workflow and are not what you would expect them to be, then it’s likely that you have mapping inaccuracies. What is data mapping, and why is it important for accurately calculating quality measure data?
CMS recently published the FY 2024 Inpatient Prospective Payment System (IPPS) Final Rule which includes several changes to the Hospital Inpatient Quality Reporting (IQR) Program and Medicare Promoting Interoperability (PI) Program for eligible hospitals (EHs) and critical access hospitals (CAHs). For the full text of the rule, see the Federal Register.
CMS recently published the FY 2024 Inpatient Psychiatric Facilities Prospective Payment System (IPF PPS) Final Rule which finalized changes to the Inpatient Psychiatric Facility Quality Reporting (IPFQR) program. All IPFs, which include psychiatric hospitals and psychiatric units of an acute care hospital or critical access hospital, paid under the IPF PPS must meet IPFQR reporting requirements. For the full text of the proposed rule, see the Federal Register.
CMS recently published the CY 2024 Quality Payment Program (QPP) Final Rule which included numerous updates to MIPS Value Pathways (MVPs) and Merit-based Incentive Payment System (MIPS). For the full text of the rule, see the Federal Register.