Effective January 1, 2023, new and revised requirements to reduce health care disparities will apply to organizations in the Joint Commission’s ambulatory health care, behavioral health care and human services, critical access hospitals, and hospital accreditation programs.
A new standard in the Leadership (LD) chapter (LD.04.03.08) with 6 new elements of performance (EPs) has been developed to address health care disparities as a quality and safety priority.
(See the full text of the requirements here R3 Report Issue 36.)
LD.04.03.08 will apply to the following Joint Commission–accredited organizations:
- All critical access hospitals and hospitals
- Ambulatory health care organizations providing primary care within the “Medical Centers” service in the ambulatory health care program (the requirements are not applicable to organizations providing episodic care, dental services, or surgical services)
- Behavioral health care and human services organizations providing “Addictions Services,” “Eating Disorders Treatment,” “Intellectual Disabilities/Developmental Delays,” “Mental Health Services,” and “Primary Physical Health Care” services
The Record of Care, Treatment, and Services (RC) requirement to collect patient race and ethnicity information has been revised and will apply to the following Joint Commission–accredited programs:
- Ambulatory health care (Standard RC.02.01.01, EP 31)
- Behavioral health care and human services (Standard RC.02.01.01, EP 26)
- Critical access hospital (Standard RC.02.01.01, EP 25)
The Rights and Responsibilities of the Individual (RI) requirement prohibit discrimination (StandardRI.01.01.01, EP 29) will apply to all Joint Commission–accredited ambulatory health care organizations, behavioral health care and human services organizations.
Requirement EP 1: Designate an individual(s) to lead activities to reduce health care disparities for the organization’s patients. Management-level leadership, physician leadership and team leadership have been consistently associated with successful quality improvement projects and is recommended
Requirement EP 2: Assess the patient’s health-related social needs and provide information about community resources and support services. Health-related social needs may be identified for a representative sample of the organization’s patients or for all the organization’s patients.
Examples of health-related social needs may include the following:
- Access to transportation
- Difficulty paying for prescriptions or medical bills
- Education and literacy
- Food insecurity
- Housing insecurity
Requirement EP 3: Identify health care disparities in the patient population by stratifying quality and safety data using the sociodemographic characteristics of the organization’s patients. Organizations may focus on areas with known disparities identified in the scientific literature. Organizations determine which sociodemographic characteristics to use for stratification analyses.
Examples of known disparities representing a sample of the organization’s patients include the following:
- Organ transplantation
- Maternal care
- Diabetes management
- Ambulatory Health Care: kidney disease, maternal care, diabetes management
- Behavioral Health Care: treatment for substance abuse disorder, restraint use, suicide rates
OR:
Examples of known disparities that affect all patients include the following:
- Experience of care and communication
Examples of sociodemographic characteristics may include the following:
- Age
- Gender
- Preferred language
- Race and ethnicity
Requirement EP 4: Develop a written action plan that describes how it will address at least one of the health care disparities identified in its patient population. The organization can then build on the lessons learned and plan to address additional disparities in the future.
The action plan should define:
- The health care disparity and the specific population(s) of focus
- The organization's improvement goal
- The strategies and resources needed to achieve the goal
- The process that will be used to monitor and report progress
Requirement EP 5: Steps to follow when goals established in the action plan are not achieved or sustained.
Examples of steps to take when goals are not achieved/sustained include the following:
- Reviewing quality and safety metrics
- Collecting feedback from patients about new services or interventions
- Evaluating staff training and education
Requirement EP 6: At least annually, inform key stakeholders (including leaders, licensed practitioners, and staff) about the progress to reduce identified health care disparities.
Record of Care, Treatment, and Services (RC) Chapter Note
Requirement: Assure that the medical records contain the patient’s race and ethnicity which will help to better understand the patient population as a whole and allow organizations to stratify key quality and safety measures to identify potential disparities in care.
Helpful Links
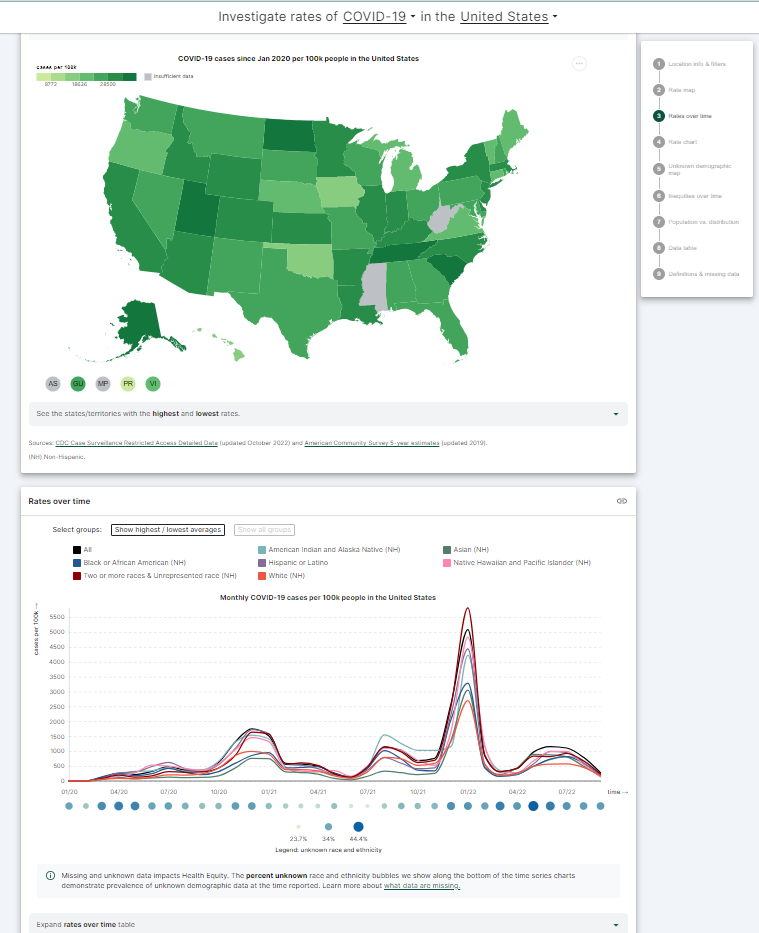
Health Equity Tracker - Designed to boost inclusivity, highlight at-risk populations, alert users to existing inequities in health data, and more.
CMS Strategic Plan - Health Equity
MEDITECH Expanse - HTN Patient Registries in Population Health Initiative
HHS Action Plan - Reduce Racial & Ethnic Health Disparities

