CMS recently published the FY 2027 Inpatient Psychiatric Facilities Prospective Payment System (IPF PPS) Proposed Rule which proposed changes to the Inpatient Psychiatric Facility Quality Reporting (IPFQR) program. All IPFs, which include psychiatric hospitals and psychiatric units of an acute care hospital or critical access hospital, paid under the IPF PPS must meet IPFQR reporting requirements. For the full text of the proposed rule, see the Federal Register.
2027 IPF PPS Proposed Rule
In this proposed rule, CMS is not proposing any new measures for the IPQQR Program. However, CMS is proposing to remove two measures beginning with the CY 2026 reporting period/FY 2028 payment determination: Alcohol Use Brief Intervention Provided or Offered (SUB-2) and subset Alcohol Use Brief Intervention (SUB-2a) measure and the Tobacco Use Treatment Provided or Offered at Discharge (TOB-3) and subset Tobacco Use Treatment at Discharge (TOB-3a) measure. CMS is proposing removal of SUB-2/SUB-2a due to the costs associated with the measure outweigh the benefit of its continued use in the program and the measure can be replaced by a more broadly applicable measure. CMS will retain the Alcohol and Other Drug Use Disorder Treatment Provided or Offered at Discharge (SUB-3) and the subset Alcohol and Other Drug Use Disorder Treatment at Discharge (SUB-3a) measure in the program since it addresses both alcohol and substance use disorder treatment in the IPF setting. CMS is also proposing removal of TOB-3/3a due to the costs associated with the measure outweigh the benefit of its continued use in the program.
CMS proposes to implement a standardized IPF patient assessment instrument (IPF-PAI) as mandated by the Consolidated Appropriations Act (CAA) of 2023. The assessment must be standardized to make meaningful comparisons across IPFs, so each IPF will administer the same assessment with identical questions, response options, standards and definitions. CMS is proposing that IPFs issue the assessment to patients aged 18 years and older.
CMS proposes the following assessment items for each of the five data categories required by the statute:
|
CAA category |
Proposed Assessment Item |
|
Functional status |
Mobility: Chair/Bed-to-Chair Transfer |
|
Cognitive function and mental status |
Suicide Screening |
|
Special services, treatments, and interventions |
Special Services, Treatments, and Interventions in the Inpatient Psychiatric Setting (Psychiatric Treatments, Restrictive Interventions) |
|
Medical conditions and comorbidities |
Primary Medical Condition Category |
|
Impairments |
Hearing; Speech Clarity; Vision |
|
Administrative: Assessment items required for record matching and database management |
Legal Name of Patient, Birth Date, Sex, Social Security and Medicare Numbers, Facility Provider Numbers (National Provider Identifier, CMS Certification Number), Admission/Discharge Date, Payer Information—Primary Payer, Type of Record, Assessment Reference Date, Reason for Assessment, Type of Admission/Type of Discharge, IPF-PAI Completion Date |
CMS is proposing to require reporting of the IPF-PAI starting with admissions and discharges for patients 18 years and older from October 1 through December 31, 2027, which impacts FY 2029 payment determination. Then, beginning with the FY 2030 payment determination, the reporting period would be the full calendar year occurring two years prior to the applicable payment year (for example, data from January 1 through December 31, 2028 would be used for FY 2030 payment determination).
The proposal also outlines that IPF-PAI data be submitted on a quarterly basis, with each quarter’s data due by the 15th day of the second month following the end of that quarter. The submission deadlines for each quarter are outlined below.
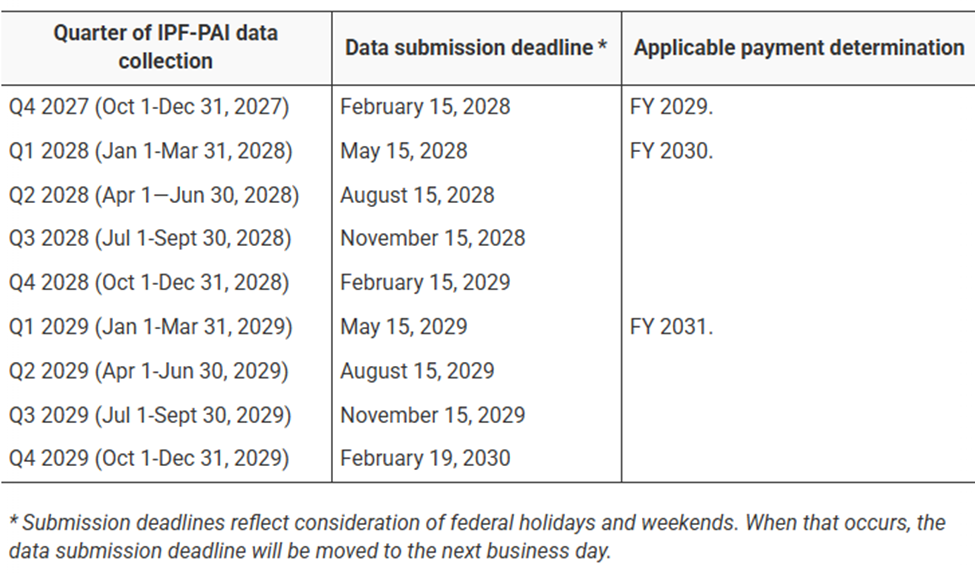
Source: CMS FY 2027 IPF PPS Proposed Rule
CMS proposes that an IPF would need to complete 100 percent of the IPF-PAI assessment items on 80 percent of the IPF-PAIs submitted to satisfy the IPF Quality Reporting Program data reporting requirements for the applicable annual payment determination. An IPF that fails to submit 100 percent of the assessment items on at least 80 percent of the IPF-PAIs submitted to CMS would be deemed non-compliant with the IPF Quality Reporting Program reporting requirements and, as a result, would be subject to a 2-percentage point reduction to its APU. In future rulemaking, CMS plans to incrementally increase the completion rate that an IPF would need to achieve to be considered compliant with the IPF Quality Reporting Program.
IPFs would be able to submit IPF-PAI data either through a CMS-developed web application or via Application Programming Interfaces (APIs) built on the Health Level Seven (HL7) Fast Healthcare Interoperability Resources (FHIR®) standard. This would mark the first CMS statutory quality reporting program to use the FHIR® standard for patient assessment data submission.
CMS has provided resources for IPF-PAI here.
If you have questions about reporting your IPFQR measures, please contact us.
