Acmeware Achieves 100% Submission Success
Featured article
Acmeware completes 100% successful submissions for eCQM, PQRS, Hospital IQR, and Joint Commission ORYX using OneView for acute and ambulatory settings.
August 15, 2023
|
Blog
Finalized IQR measure changes, eCQM additions, and mandatory SAFER Guides attestation
The FY 2024 IPPS Final Rule confirms changes to the Hospital IQR and Medicare PI programs for eligible hospitals and CAHs.
CMS recently published the FY 2024 Inpatient Prospective Payment System (IPPS) Final Rule which includes several changes to the Hospital Inpatient Quality Reporting (IQR) Program and Medicare Promoting Interoperability (PI) Program for eligible hospitals (EHs) and critical access hospitals (CAHs). For the full text, see the Federal Register.
CMS finalized numerous changes including the adoption of three new measures, the refinement of three existing measures and the removal of three measures.
CMS finalized three new eCQMs available for self-selection beginning with CY 2025 reporting period/ FY 2027 payment determination.
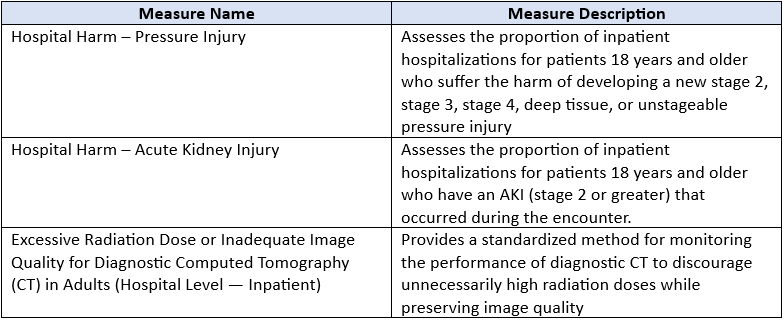
CMS finalized modifications to three existing measures and the HCAHPS survey measure.

CMS finalized the removal of three measures.

CMS finalized that beginning with CY 2024 reporting period, EHs and CAHs are required to attest "yes" to having conducted an annual self-assessment of all nine SAFER Guides at any point during the calendar year in which the EHR reporting period occurs.
CMS also finalized adoption of three new eCQMs for self-selection beginning with CY 2025 in alignment with IQR:
For questions about hospital reporting, please contact us.