Acmeware Achieves 100% Submission Success
Featured article
Acmeware completes 100% successful submissions for eCQM, PQRS, Hospital IQR, and Joint Commission ORYX using OneView for acute and ambulatory settings.
July 20, 2022
|
Blog
Proposed updates to MIPS and five new MIPS Value Pathways
The CY 2023 QPP Proposed Rule outlines updates across all four MIPS performance categories and introduces new MVPs.
CMS recently published the CY 2023 Quality Payment Program (QPP) Proposed Rule featuring numerous updates to MIPS Value Pathways (MVPs) and Merit-based Incentive Payment System (MIPS). For comprehensive details, see the Federal Register.
CMS continues advancing MIPS Value Pathways to improve value, reduce burden, inform patient choice in selecting clinicians, and reduce barriers to participation in Alternative Payment Models (APMs).
The 5 newly proposed MVPs for 2023 are:
The 2023 MIPS score continues using four performance categories with a 75-point threshold.
CMS proposes 194 quality measures for 2023, adding 9 new measures including administrative claims measures, composite measures, high-priority measures, and patient-reported outcome measures.
A maximum 1 percentage point improvement score is established for the cost category.
Four new improvement activities are proposed, with 5 modified and 6 removed.
Beginning 2023, automatic reweighting discontinues for nurse practitioners, physician assistants, certified registered nurse anesthetists, and clinical nurse specialists.
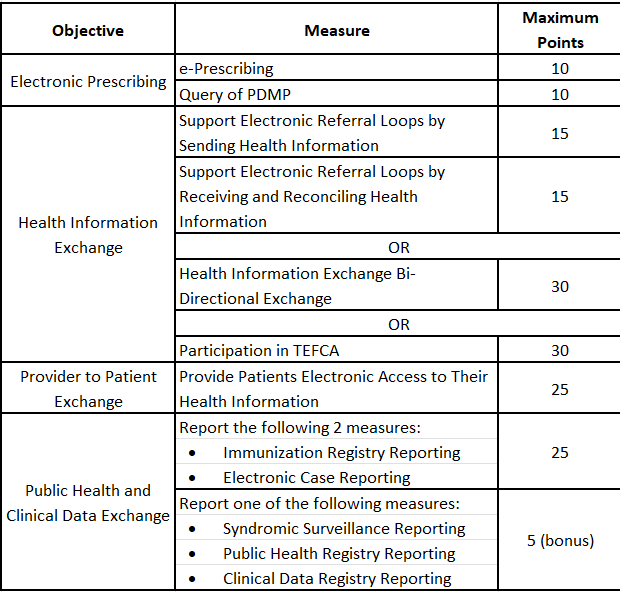
The Public Health and Clinical Data Exchange Objective reduces from 3 to 2 engagement levels. The Query of PDMP becomes required (worth 10 points), expanding to include Schedules III and IV drugs. A third option, Participation in TEFCA, is proposed for the HIE Objective.
For questions about MIPS/MVPs reporting, contact Acmeware.