Acmeware Achieves 100% Submission Success
Featured article
Acmeware completes 100% successful submissions for eCQM, PQRS, Hospital IQR, and Joint Commission ORYX using OneView for acute and ambulatory settings.
November 16, 2022
|
Blog
Finalized updates to MIPS scoring, quality measures, and Promoting Interoperability
The CY 2023 QPP Final Rule confirms updates across all MIPS performance categories and expands the MVP framework.
CMS recently published the CY 2023 Quality Payment Program (QPP) Final Rule which included numerous updates to MIPS Value Pathways (MVPs) and Merit-based Incentive Payment System (MIPS). For the full text of the rule, see the Federal Register.
CMS finalized 5 new MVPs and revised the 7 previously established MVPs available beginning with the 2023 performance year:
CMS also finalized changes for subgroup reporting to MVPs, including requirements for TIN/NPI lists, plain language names, and composition descriptions. Subgroups would receive affiliated group scores for Foundational Layer measures and outcome-based administrative claims measures.
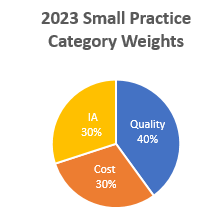
For 2023 MIPS reporting, the MIPS score continues to be based on the four performance categories and their corresponding weights. CMS finalized that clinicians and groups must continue to reach a minimum of 75 points to avoid a negative payment adjustment in 2025. Additionally, clinicians will no longer have an additional threshold for exceptional performance bonus in 2023.

CMS finalized a total of 198 measures for the 2023 performance period, adding 9 quality measures. 11 quality measures were finalized for removal, and 2 were removed from MIPS but retained in MVPs.


CMS finalized that administrative claims measures will be scored using performance period benchmarks, while quality measures continue using historical benchmarks. Data completeness remains at 70% for 2023, increasing to 75% for 2024 and 2025.
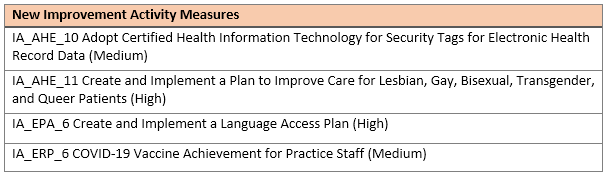
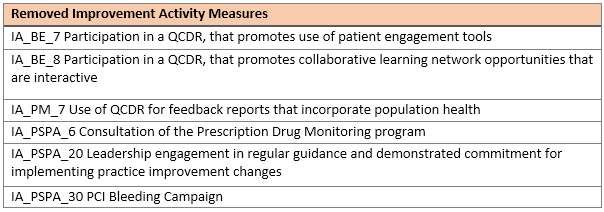
CMS finalized updates to the improvement activities inventory by adding 4 new, modifying 5, and removing 6.
Beginning with 2023, CMS finalized discontinuing automatic reweighting of PI for nurse practitioners, physician assistants, certified registered nurse anesthetists, and clinical nurse specialists.
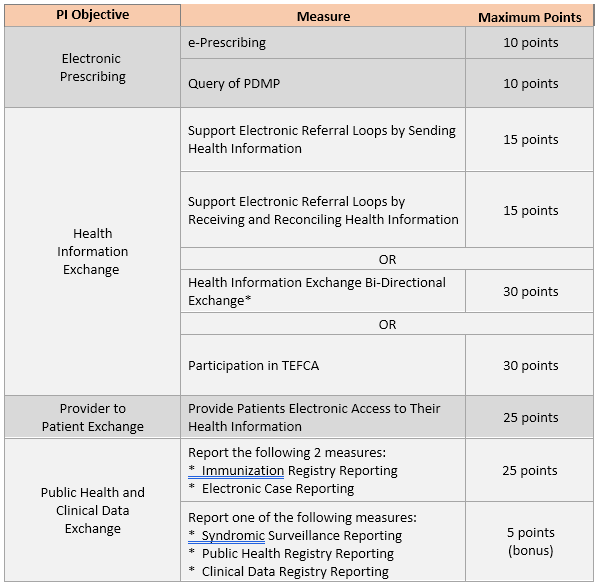
CMS finalized reducing active engagement levels from 3 to 2 by combining Options 1 and 2 into "Pre-production and Validation" and renaming Option 3 to "Validated Data Production."
The Query of PDMP becomes required (10 points), expanded to include Schedules III and IV drugs. CMS finalized a 3rd option for the HIE Objective: Participation in TEFCA.
CMS finalized a maximum cost improvement score of 1 percentage point out of 100 percentage points for the cost performance category.
For MIPS/MVPs reporting questions, please contact us.